In the complex landscape of metabolic health, numbers serve as the language of the body. For anyone navigating the confusing waters of blood sugar management—whether you are newly diagnosed, a long-term diabetic, or simply health-conscious—there is one acronym that reigns supreme: HbA1c.
In this detailed guide, we will decode the science of HbA1c, explain why it is the global gold standard for diagnosis, and provide actionable strategies to master your metrics.
The Science Behind the Number: What is HbA1c?
To understand the test, we have to look microscopically at your blood. “Hb” stands for Hemoglobin, the protein found within your red blood cells (RBCs) responsible for carrying oxygen from your lungs to the rest of your body. “A1c” refers to a specific subtype of hemoglobin that has a peculiar affinity for glucose.
Here is the mechanism: Glucose (sugar) circulates in your bloodstream. When that glucose bumps into hemoglobin, it sticks to it. This process is called glycation. Think of it like a sugar-glazed donut; once the sugar coats the donut, it doesn’t come off. Similarly, once glucose attaches to hemoglobin, it stays there for the entire lifespan of that red blood cell.

This biological mechanism is why the HbA1c is often referred to as the “lie detector” of diabetes management. You can “cheat” a fasting blood sugar test by eating strictly for 24 hours prior to the lab visit, resulting in a normal morning reading. However, you cannot fool the HbA1c. It captures every spike, every cheat meal, and every stress-induced rise in glucose over the last quarter of the year.
Why Is This Test the “Gold Standard”?
For decades, the fasting plasma glucose test was the primary method for diagnosing diabetes. However, relying solely on fasting levels can be misleading due to the “Dawn Phenomenon” (a natural morning spike in hormones) or temporary dietary changes.
The HbA1c has become the preferred diagnostic tool for several reasons:
- Convenience: Unlike fasting tests, the HbA1c does not require you to starve yourself overnight. You can have the blood drawn at any time of day, making it easier for patients to comply with testing schedules.
- Stability: It is less likely to be affected by temporary factors like acute stress or a recent viral illness compared to a standard blood glucose test.
- Risk Prediction: Perhaps most importantly, the HbA1c number directly correlates with the risk of long-term complications. Extensive clinical studies have shown that for every 1% drop in HbA1c, the risk of microvascular complications (like eye, kidney, and nerve disease) drops by nearly 40%.
If you have been monitoring your health but find that your numbers remain inconsistent, it is vital to stop guessing and start consulting with a specialist who looks at the big picture. Seeking guidance from the Best diabatologist in Coimbatore can help you interpret these long-term trends rather than just reacting to daily fluctuations.
Decoding the Ranges: What Do Your Numbers Actually Mean?
Understanding your HbA1c result is the first step toward taking control. The results are reported as a percentage, representing the proportion of your hemoglobin that is glycated.
Global adult diabetes prevalence ~ 9% with forecasts projecting a large increase by 2035
1. The Normal Range (Below 5.7%)
If your result is below 5.7%, your metabolic health is considered optimal. It means your body is producing adequate insulin and your cells are responding to it efficiently, keeping glucose from accumulating in the blood.
2. Pre-Diabetes (5.7% to 6.4%)
This is the critical “warning zone.” A reading in this range indicates that your average blood sugar is higher than normal, but not yet high enough to be classified as full-blown diabetes.
- The Reality Check: Most people with pre-diabetes do not have symptoms. Without intervention, a significant percentage of people in this range will develop Type 2 diabetes within 5 to 10 years. However, this is also the stage where lifestyle changes are most effective at reversing the trajectory.
3. Diabetes (6.5% and Above)
An HbA1c level of 6.5% or higher, confirmed on two separate occasions, is the diagnostic threshold for diabetes.
- The Target: If you are already diagnosed with diabetes, the goal shifts. For most adults, the American Diabetes Association recommends aiming for an HbA1c below 7%. However, this target is not rigid. Younger patients might aim for 6.5% to prevent long-term damage, while elderly patients might have a looser target (around 8%) to avoid the dangers of hypoglycemia (dangerously low blood sugar).
The Hidden Dangers: Why High HbA1c Matters
Over time, this sugar-laden blood damages the delicate inner lining of your blood vessels. This damage manifests in three primary areas:
- Retinopathy: Damage to the tiny blood vessels in the eyes, potentially leading to blindness.
- Nephropathy: Damage to the filtering units of the kidneys, which can lead to kidney failure and the need for dialysis.
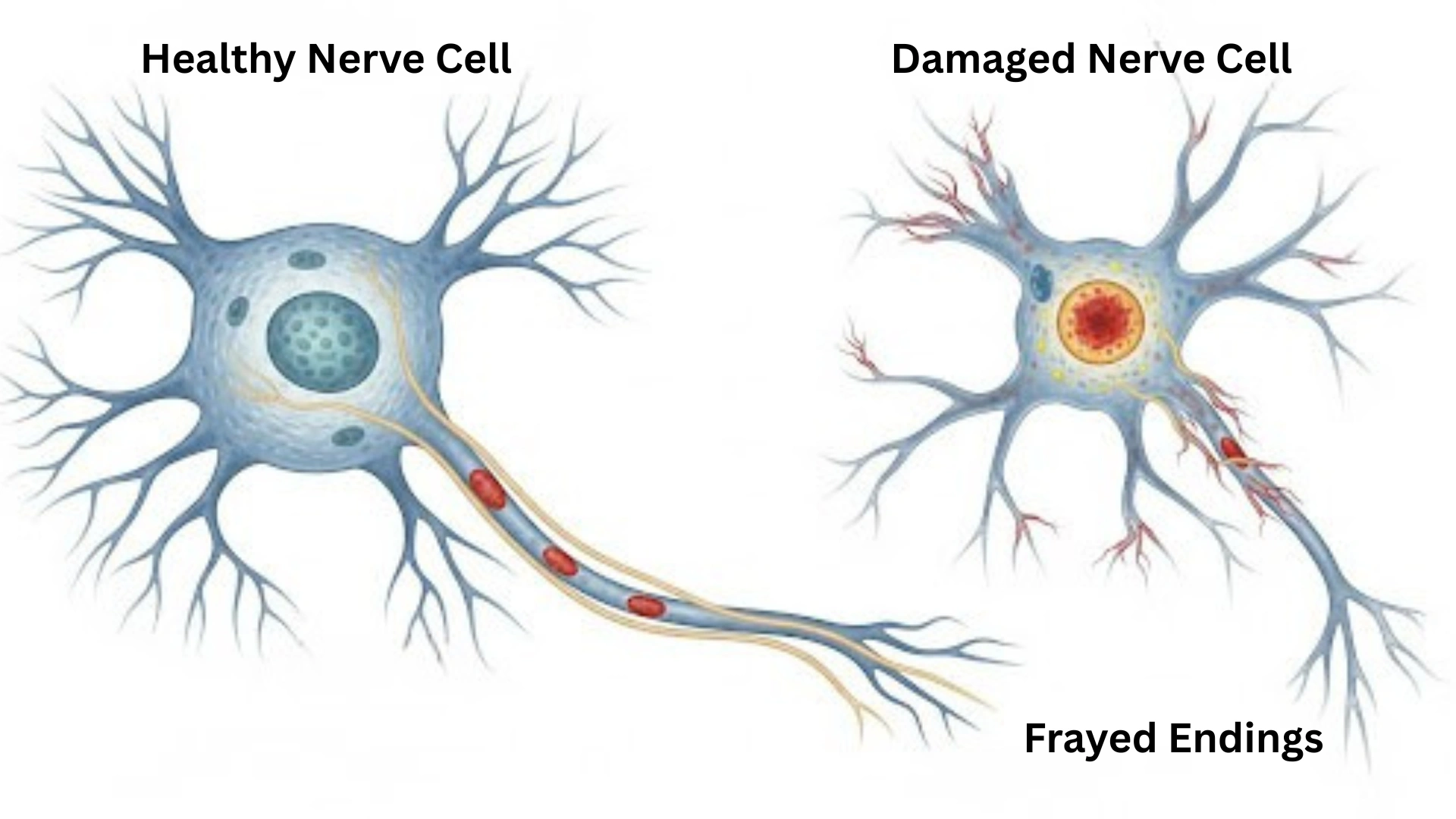
- Neuropathy: Damage to the nerves, particularly in the feet and hands, leading to loss of sensation, pain, and increased risk of amputation from unnoticed injuries.
Strategies for Improvement: How to Lower Your HbA1c
If your diagnostic report shows an elevated HbA1c, do not panic. This metric is dynamic. With the right interventions, you can lower your score significantly in just 3 to 6 months.
1. Nutrition: The Glycemic Index Approach
You cannot out-medicate a bad diet. The most effective way to lower HbA1c is to control the input of glucose.
- Focus on Fiber: Soluble fiber (found in oats, flaxseeds, and legumes) forms a gel-like substance in the gut, which slows down the absorption of sugar into the bloodstream.
- Watch the Carbohydrate Load: It is not just about avoiding “sweets.” White rice, white bread, and potatoes convert to sugar rapidly. Switching to complex carbs like quinoa, brown rice, and whole wheat prevents the sharp spikes that drive up your average.
Also read: Early Kidney Damage Symptoms and Prevention
2. Physical Activity: The Insulin Sensitizer
Exercise acts like a “backdoor” for glucose. When you exercise, your muscles need energy and will pull glucose directly from the bloodstream, even without the help of insulin.
- Resistance Training: Building muscle is particularly beneficial because muscle tissue burns more glucose at rest than fat tissue does.

3. Stress and Sleep Hygiene
Chronic stress triggers the release of cortisol and adrenaline. These “fight or flight” hormones signal the liver to dump extra sugar into the bloodstream to provide energy for the perceived threat. If you are stressed but sedentary, that sugar just sits in your blood, raising your HbA1c. Prioritizing 7-8 hours of sleep and practicing mindfulness can have a surprising impact on your blood test results.
This is where a holistic approach becomes non-negotiable. You need a medical partner who understands that diabetes is a 24/7 condition. Opting for comprehensive Diabetes Treatment in Coimbatore ensures that you are not just receiving a prescription, but a complete management plan that includes dietary counseling, foot care, and regular monitoring to keep complications at bay.
Empowering Yourself Through Data
The HbA1c test is more than a diagnostic requirement; it is a tool for empowerment. It strips away the denial that often comes with chronic illness and provides a clear, undeniable picture of your metabolic status.
By understanding what this number represents, you move from being a passive patient to an active CEO of your own health. Whether you are working to reverse pre-diabetes or managing a lifelong condition, the goal remains the same: stability, consistency, and awareness.
Take the time to discuss your target range with your doctor. Review your diet honestly. commit to movement, and seek out the best medical support available. Your health is a long-term investment, and understanding your HbA1c is the best way to ensure that investment yields a long, healthy life.