Blackening of Legs in Diabetics: Causes, Symptoms, and Effective Treatments
For many people living with diabetes, noticing dark or black patches on the legs can be alarming. The first thought that often comes to mind is, “Is this serious?” or “Could this lead to complications like gangrene or amputation?” While leg blackening can be a sign of poor circulation or other underlying issues, it’s important to understand that not all causes are dangerous. Some are harmless and reversible with proper care, while others require urgent medical attention.
Dr. Arun Karthik, the best diabetologist in Coimbatore, emphasizes that while some causes are minor and manageable, others can pose serious risks if ignored. Early detection, proper diabetes management, and timely medical intervention are crucial to maintaining healthy legs and preventing complications.
In this guide, we will explore the five primary causes of leg blackening in diabetic patients, explain how to recognize them, and discuss effective management and treatment strategies.
Diabetic Shin Spots (Hyperpigmented Dermatopathy)

What it is
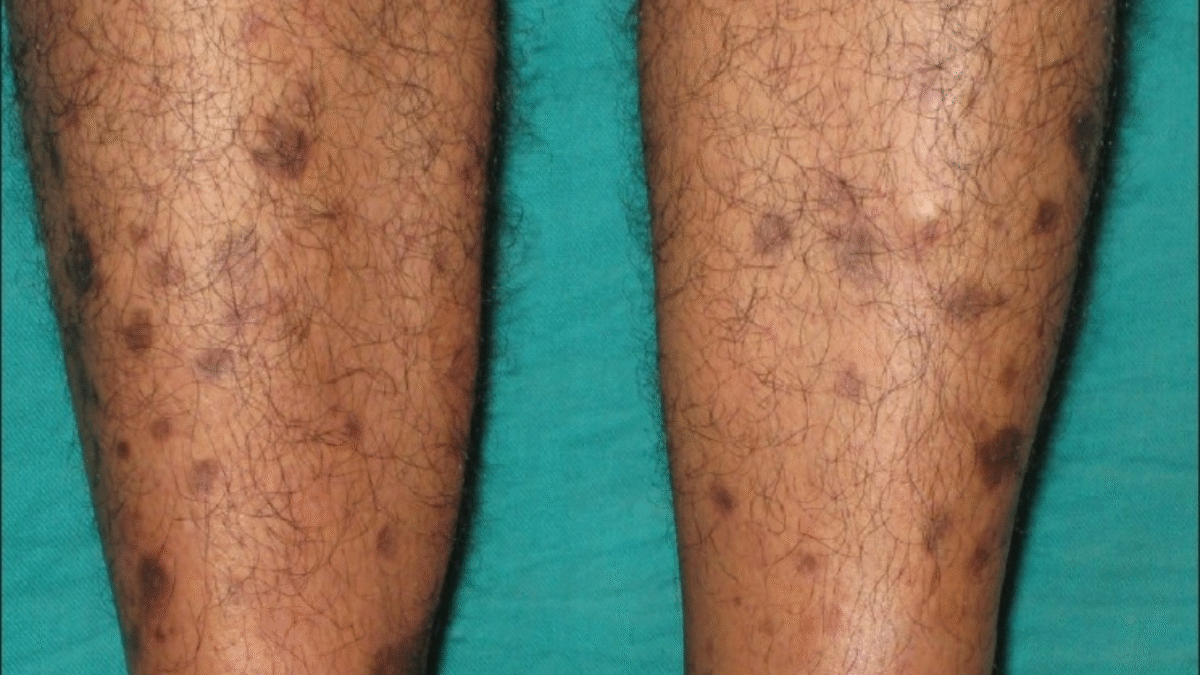
One of the most common and least concerning causes of leg darkening in diabetic patients is Diabetic Dermopathy, also known as Shin Spots. These spots typically appear on the front of the lower legs, below the knees. They are small, round, brown or black patches, often likened in size to a small coin or a forehead bindi.
Why it happens
Diabetic dermopathy is linked to long-term high blood sugar levels, which can damage the small blood vessels and nerves in the skin. Minor injuries, such as bumps or knocks, can also trigger these spots. It is important to note that these spots are painless, non-itchy, and do not usually indicate a serious underlying problem.
People with diabetes for over 10 years are more likely to develop these spots, and they may appear in clusters or in a linear pattern along the shin.
Symptoms
- Small, round brown or black spots on the lower legs
- No pain, burning, or itching
- May appear more after minor injuries
Treatment
There is no specific medical treatment required for diabetic shin spots. The key is maintaining optimal blood sugar control, which helps these marks gradually fade over time. Regular skincare, avoiding injuries, and keeping the legs moisturized can prevent new spots from forming.
While these spots can look alarming, they are generally harmless and are often the first sign of long-term diabetes-related skin changes.
Xerotic Eczema (Dry Skin or Xerotic Dermatitis)
What it is
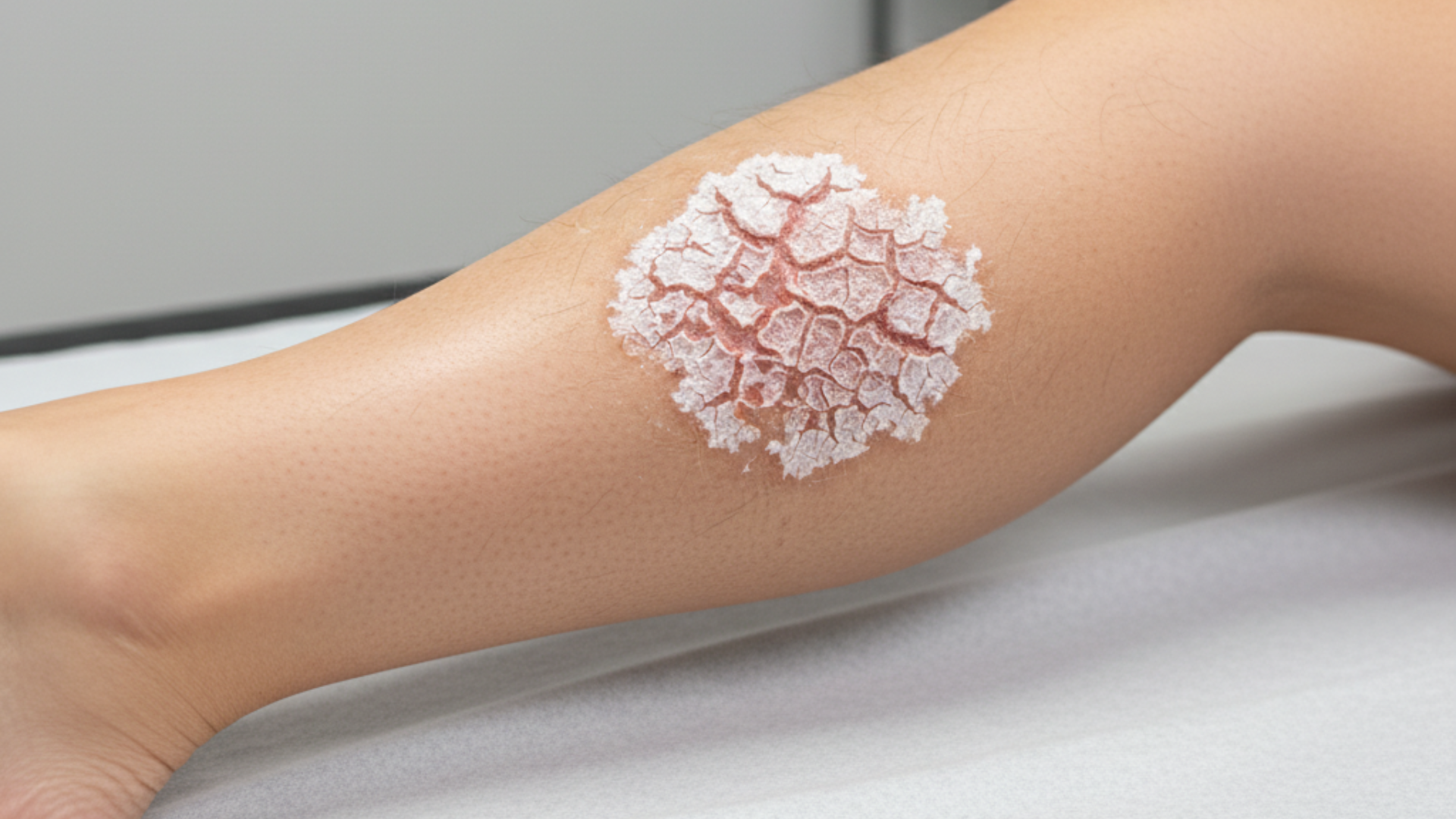
As people age, especially those with diabetes, the skin tends to become dry and flaky. This condition, known as Xerotic Eczema, can make the legs appear dark, rough, and scaly, resembling fish scales or peeling paint. Xerotic eczema is not only a cosmetic issue; it can cause discomfort and intense itching, which may interfere with daily life.
Why it happens
In diabetes, the oil glands in the skin produce less sebum, the natural oil that keeps the skin hydrated. This reduction in natural oils, combined with poor circulation and dehydration, leads to dry, rough, and sometimes cracked skin, particularly below the knees. Dryness tends to worsen during cold or dry seasons and can become severe if left untreated.
Symptoms
- Dry, rough, or scaly skin
- Itchy patches, especially in the evenings
- Powdery white flakes mixed with darkened areas
- Cracked skin that may be prone to minor infections
Treatment
- Apply oil-based moisturizers or emollients daily to restore hydration
- Use mild, fragrance-free soaps and avoid hot showers, which strip the skin of oils
- Take anti-itch medications if necessary
- Keep the skin protected with comfortable clothing and avoid scratching
While xerotic eczema is generally not dangerous, persistent dryness can increase the risk of skin infections. Maintaining proper hydration, skincare, and blood sugar control can prevent complications.
Venous Stasis Ulcer
What it is
Venous Stasis Ulcers are more serious than shin spots or xerotic eczema. They occur when blood pools in the veins of the lower legs due to weak or damaged vein valves. This condition, also referred to as Chronic Venous Insufficiency, often results in darkened skin, swelling, and in severe cases, open sores (ulcers).
Why it happens
The veins in our legs contain one-way valves that help blood flow back to the heart. When these valves weaken or fail, blood begins to pool in the lower legs, increasing pressure and causing the skin to darken. Over time, iron from red blood cells leaks into the skin, creating a brown or black pigmentation known as Hemosiderosis.
Diabetic patients are more prone to venous stasis ulcers because long-term high blood sugar can damage veins and affect circulation. Standing or walking for extended periods further aggravates the condition.
Symptoms
- Swelling, heaviness, or aching in the legs
- Dark brown or black patches on the lower legs
- Itching or throbbing pain, particularly at night
- Thickened skin or open ulcers in advanced cases
- Visible twisted or bulging veins (varicose veins)
Treatment
- Compression stockings improve blood flow and reduce swelling
- Elevating the legs above heart level several times a day
- Regular exercise to stimulate circulation
- Surgical or vascular interventions in severe cases with ulcers
Early intervention can prevent progression to painful ulcers and reduce the risk of infections or chronic wounds.
Kyrle’s Disease (Acquired Perforating Dermatosis)
What it is
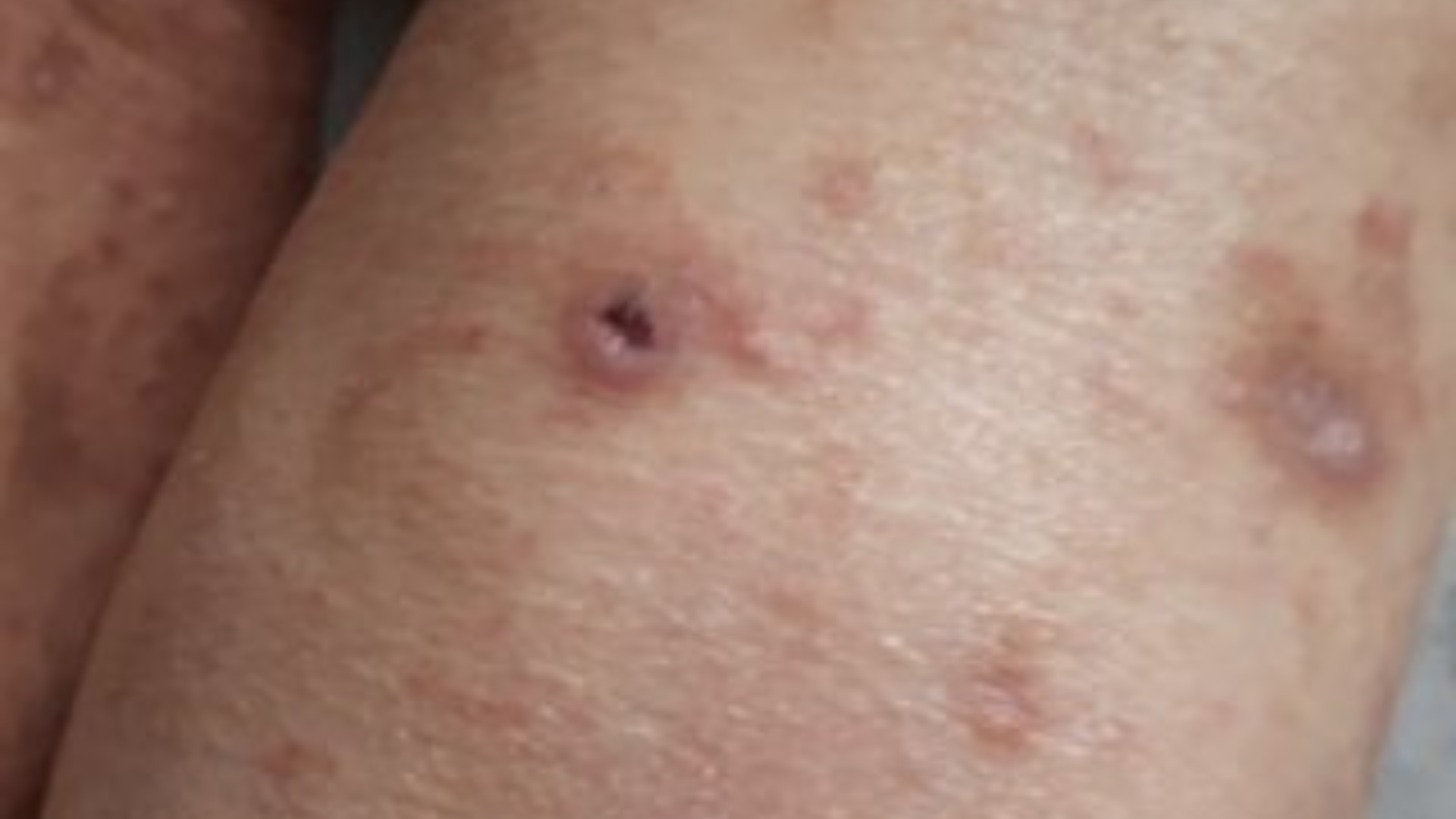
Kyrle’s Disease, or Acquired Perforating Dermatosis, is a less common cause of leg blackening. It usually occurs in diabetic patients with kidney disease. This condition appears as dark circular spots with white centers, and it is often accompanied by intense itching and discomfort.
Why it happens
Kyrle’s Disease is linked to impaired kidney function. When the kidneys fail to remove toxins effectively, waste products build up in the body and trigger inflammatory skin reactions, resulting in black, itchy lesions. This condition is most common in people with chronic kidney disease or those undergoing dialysis.
Symptoms
- Small, dark spots with raised white centers
- Severe, persistent itching
- Skin may become thickened and rough over time
- Often affects both legs symmetrically
Treatment
- Managing the underlying kidney problem is crucial
- Use anti-itch medications and oil-based moisturizers to reduce discomfort
- Control blood sugar and blood pressure to prevent worsening symptoms
- Avoid scratching to prevent infections
Although Kyrle’s Disease can be persistent, proper treatment of kidney and diabetic issues can significantly reduce symptoms and improve quality of life.
Peripheral Arterial Disease (PAD) – The Most Dangerous Cause
What it is
Among all causes of leg blackening, Peripheral Arterial Disease (PAD) is the most serious. PAD occurs when the arteries that carry oxygen-rich blood from the heart to the legs become narrowed or blocked. Reduced blood flow means that tissues don’t get enough oxygen, which can lead to pain, blackened skin, tissue death, and gangrene if left untreated.
Why it happens
PAD is primarily caused by atherosclerosis, a buildup of fatty deposits inside the arteries. Diabetics, people with high cholesterol, and smokers are at much higher risk. Smoking, in particular, accelerates arterial damage and worsens circulation problems.
Symptoms
- Pain in the calves while walking (called claudication pain), relieved by rest
- Cold, pale, or numb feet
- Non-healing wounds or ulcers on the toes or feet
- Blackened areas indicating tissue death
- Progressive leg pain, even at rest, in advanced stages
Treatment
- Seek medical attention immediately if you notice blackened areas or non-healing wounds
- Diagnostic tests such as Doppler scans or angiograms to assess blood flow
- Lifestyle changes: quit smoking, control cholesterol, maintain blood sugar
- Medications to improve circulation and prevent blood clots
- Surgical procedures, including angioplasty or bypass surgery, may be necessary in severe cases
When to See a Doctor
Leg blackening, persistent swelling, or pain should never be ignored. According to Dr. Arun Karthik at Diacare Centre in Coimbatore, diabetic patients should consult a doctor promptly if they notice:
- Dark or black patches that do not fade
- Non-healing wounds, sores, or ulcers on the feet or toes
- Severe itching or discomfort that does not improve with moisturizers
- Cold, numb, or pale feet indicating poor circulation
Timely medical evaluation at a specialized center like Diacare ensures proper diagnosis and treatment, helping to prevent serious complications such as gangrene or amputation.
Also Read: Ten Everyday Foods to Help Control Diabetes Naturally
Preventing Leg Blackening in Diabetics
While some causes of leg blackening are unavoidable with long-term diabetes, many can be prevented or managed through consistent care:
- Maintain optimal blood sugar levels through medication, diet, and exercise.
- Moisturize daily to prevent dryness and itching.
- Wear comfortable, protective footwear to prevent injuries.
- Avoid smoking, which damages blood vessels.
- Regularly check your legs and feet for changes in skin color, swelling, or wounds.
- Elevate your legs when sitting to improve circulation.
- Exercise regularly to support vascular health.
By combining good diabetic control with careful skin and vascular care, patients can significantly reduce the risk of serious leg complications.
Conclusion
Leg blackening in diabetics can arise from a range of causes — from harmless skin changes to serious vascular complications. The key to prevention and treatment lies in early detection, proper blood sugar management, skincare, and timely medical intervention.
Mild conditions like diabetic shin spots and xerotic eczema are generally harmless and improve with routine care. Conditions such as venous stasis ulcers, Kyrle’s Disease, and Peripheral Arterial Disease (PAD) require more intensive care and, in some cases, urgent attention.
Regular monitoring, proper skincare, and expert diabetes treatment in Coimbatore from specialists like Dr. Arun Karthik at Diacare Centre, will help diabetic patients maintain healthy, strong legs and prevent serious complications, allowing them to stay mobile and independent.