Four Diabetes-Linked Nerve Issues You Must Know Today
Living with diabetes requires a constant balancing act between diet, medication, and lifestyle choices. While most people associate high blood sugar primarily with energy crashes or kidney concerns, one of the most insidious and widespread complications is nerve damage, medically known as diabetic neuropathy. High blood glucose levels, over time, act as a slow-acting toxin to the delicate nervous system, injuring the nerves throughout the body. This damage can range from mild numbness to debilitating pain and can affect the function of internal organs. For individuals navigating this chronic condition, finding the right medical guidance is paramount. If you are currently seeking Diabetes Treatment in Coimbatore, it is essential to understand that managing your sugar levels is the primary defense against the progression of these nerve disorders.
Unveiling the Silent Damage and Specific Nerve Conditions
Nerve damage does not manifest in the same way for every patient. The symptoms depend entirely on which nerves are affected. In the medical community, these are generally categorized into four distinct types, each presenting its own set of challenges. Understanding these categories helps in early identification, which is the key to preventing irreversible damage.
The first and most common form is Peripheral Neuropathy. This type primarily affects the feet and legs, followed by the hands and arms. It often starts softly, with a sensation that many patients describe as “walking on cotton bed” or wearing socks when they are barefoot. As it progresses, symptoms become more aggressive. Patients may experience tingling, burning sensations, sharp or stabbing pains, and eventually, a complete loss of feeling. The danger here lies in the numbness; a person might step on a sharp object or a hot sun scorched surface( like in temples), develop a blister, or suffer a minor injury without realizing it. Because diabetes also affects blood flow, these unnoticed injuries can become infected and lead to serious complications like ulcers or, in severe cases, amputation. The loss of temperature sensitivity is also a major risk factor, as patients may unknowingly burn themselves with hot water.
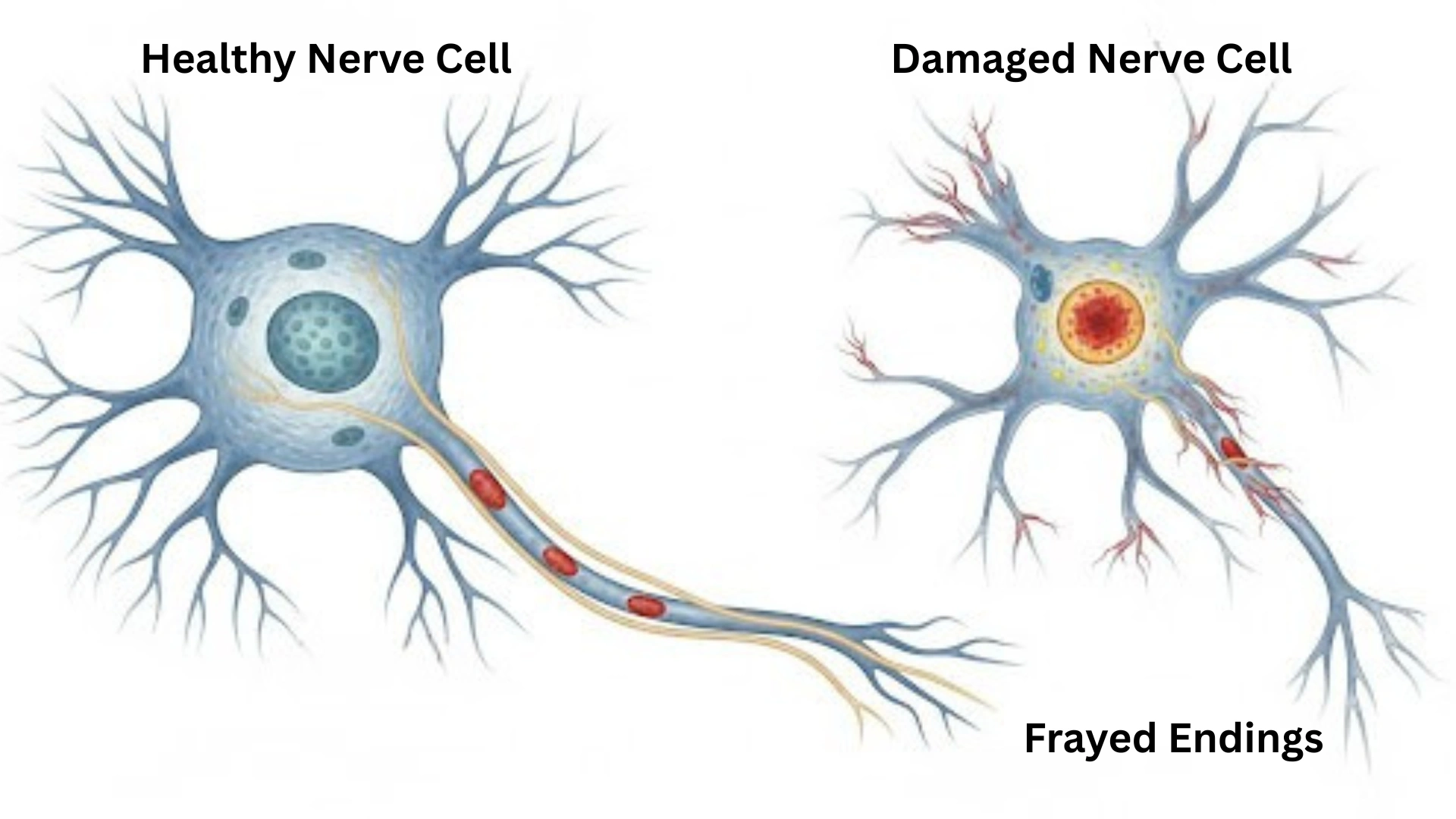
The second major category is Autonomic Neuropathy. Unlike peripheral neuropathy which affects what you feel, this type affects what your body does automatically. The autonomic nervous system controls your heart, bladder, stomach, intestines, sex organs, and eyes. When diabetes damages these nerves, the body’s internal regulation goes haywire. Digestive issues are common, leading to a condition called gastroparesis, where the stomach empties too slowly, causing nausea, vomiting, and bloating. It can also mask the symptoms of low blood sugar, a phenomenon known as hypoglycemia unawareness, which can be dangerous especially in elderly. Cardiovascular issues may arise, such as a racing heart rate even at rest, or a sudden drop in blood pressure when rising from a sitting position, causing dizziness or fainting. Bladder problems, including retention or incontinence, are also frequent complaints associated with this type of nerve damage.
The third type is often referred to as Proximal Neuropathy, also known as diabetic amyotrophy. This is less common than peripheral neuropathy and affects the nerves in the thighs, hips, buttocks, or legs. It typically affects older adults and often impacts only one side of the body, though it can spread to the other. The symptoms are usually sudden and severe. Patients report deep, intense pain in the hip or thigh, followed by eventual weakness in the thigh muscles. This can lead to a noticeable shrinking of the muscle tissue and difficulty rising from a sitting position without assistance. While peripheral neuropathy is a gradual decline, proximal neuropathy often feels like a sudden attack on the body’s structural integrity, making mobility difficult and painful.
Also Read : Type Five Diabetes Classification and Treatment
The fourth category is Focal Neuropathy, or mononeuropathy. As the name suggests, this involves damage to a specific, single nerve. It can appear suddenly and affect a nerve in the head, torso, or leg. This might manifest as double vision, aching behind one eye, paralysis on one side of the face (Bell’s palsy), or severe pain in the lower back or pelvis. One of the most well-known forms of focal neuropathy is carpal tunnel syndrome, where the median nerve in the wrist is compressed. While focal neuropathy can be intensely painful and frightening due to its sudden onset, the positive aspect is that it usually does not cause long-term damage. With time and proper management, symptoms often resolve on their own over weeks or months, unlike the chronic progression of peripheral neuropathy.
Globally, pooled estimates of painful diabetic peripheral neuropathy (PDPN) — i.e. neuropathy with pain symptoms — is ~ 46.7% (95% CI 41.8–51.7%) among those with DPN.
Comprehensive Approaches to Treatment and Long-Term Care
While the description of these nerve problems can be alarming, the focus must always shift toward management and treatment. There is currently no cure that can reverse the nerve damage once it has occurred, which is why the primary goal of treatment is twofold: slowing the progression of the disease and managing the symptoms to improve quality of life.
The cornerstone of all treatment plans is the strict regulation of blood glucose levels. Keeping blood sugar within the target range is the only way to stop the toxic effect on the remaining healthy nerves. This often involves a combination of oral medications, insulin therapy, and rigorous monitoring. Consistent blood sugar control can surprisingly reduce some neuropathic symptoms and is the most effective way to prevent further deterioration. Alongside glucose control, managing blood pressure and cholesterol is vital, as good circulation is required to feed the nerves and help them repair where possible.
Pain management is the second pillar of treatment. Regular painkillers found over the counter often do not work for nerve pain. Instead, physicians prescribe specific medications originally developed for other conditions but found effective for neuropathy. These include anti-seizure medications and certain antidepressants. These drugs work by interfering with the chemical processes in the brain and spinal cord that cause you to feel pain. Topical treatments, such as creams containing capsaicin, can also provide localized relief for burning sensations. It is crucial to have an open dialogue with healthcare providers to find a medication regimen that offers relief without unmanageable side effects.

Lifestyle modifications play a massive role in treatment efficacy. Vitamin deficiencies, particularly B12, can mimic or worsen neuropathy, so a diet rich in essential nutrients is non-negotiable. Foods high in antioxidants, lean proteins, and whole grains support nerve health. Exercise is equally critical; even light activities like walking or swimming can improve blood flow to the limbs and help keep blood sugar levels stable. However, those with significant foot numbness must choose low-impact exercises to avoid injuring their feet. Smoking is perhaps the biggest enemy of diabetic neuropathy because it constricts blood vessels, depriving nerves of nutrients and oxygen. Quitting smoking is often the single most impactful lifestyle change a patient can make.
Finally, daily self-care rituals are the best defense against severe complications. This includes inspecting feet every day for cuts, blisters, or red spots. Using a mirror to check the bottoms of the feet or asking a family member for help can save a limb. Keeping skin moisturized to prevent cracking, wearing well-fitting shoes, and avoiding walking barefoot are simple habits that provide a layer of protection against the loss of sensation.
Nerve damage is a serious complication, but it does not have to dictate the entirety of one’s life. With early detection, strict sugar control, and a proactive approach to physical health, the progression can be halted. It requires a partnership between the patient and their healthcare team. If you are experiencing tingling, pain, or any unusual symptoms, do not wait for them to worsen. Immediate intervention is key. For specialized care and a comprehensive management plan tailored to your needs, it is highly recommended to consult a best Sugar doctor in coimbatore who can guide you toward a pain-free and healthier future.